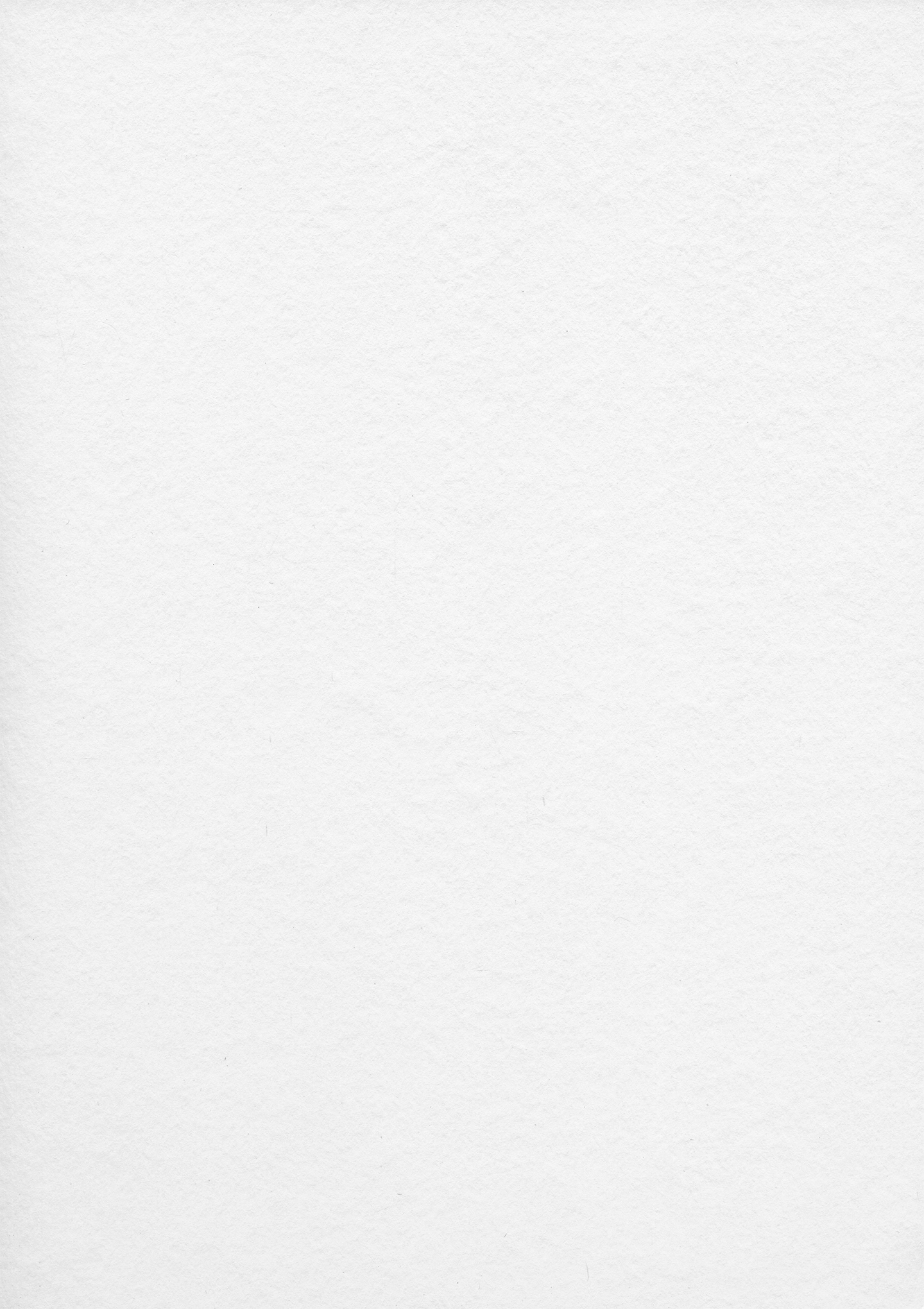Brooke Garner has rheumatoid arthritis, she’s been diagnosed with thyroid cancer, and she experiences ongoing autoimmune attacks. Any of these health struggles would be enough for a lifetime, but Garner is only in her 20s. Unfortunately, this also means she’s learned the hard way how difficult, expensive, and opaque the American healthcare system has become.

“It first started when I was four,” Garner told IW Features. “I actually got scarlet fever… It is a form of strep.”
“Very soon after, I started breaking out in hives everywhere,” she continued. “[My parents] took me to an immunologist… They did blood work, and it came back positive, saying I had high ANA [antinuclear antibodies] and rheumatic factor.”
Simple allergy medications made the hives subside, Garner explained, but the doctors suggested that she could develop more symptoms in the future.
Initially, she seemed to be in the clear. Then, when she turned 14, her life turned upside down.
“I hit puberty, and I started getting extreme migraines and just pain everywhere,” she said.
She said she missed school and struggled to eat because the pain was centralized in her jaw joint. She went to an oral surgeon and got a scan of her jaw, but left without answers. Garner said that doctors doubted her, suggesting her pain was fake.
“I was told first when I was 14 that I was looking for opioids and attention by the first rheumatologist I went to go see,” she said.
Eventually, her mother took her to the hospital and wouldn’t leave until a doctor would do an exploratory procedure, according to Garner. She said the procedure revealed that she had an autoimmune disease, though she didn’t know what kind—or how to treat it.
“Autoimmune, rheumatoid disorders, they can be very hard to diagnose,” she explained.
Still only a teenager, Garner had already gone through multiple jaw surgeries and, still in pain, asked for a complete joint replacement.
“I got my jaw joint placed at 16,” she said. “It was my junior year of high school, and that was a complete turnaround for me.”
She’d missed so much of her high school experience due to her chronic health battles, but the joint replacement let her finally live with less pain, go back to school, and play sports.
Meanwhile, she said she was in a confusing back-and-forth with insurance coverage. Despite the jaw surgeries and replacement being related to arthritis, she said the health insurance company was claiming the procedures were dental or cosmetic—which are typically not covered by health insurance.
Then, the autoimmune disease—possibly caused by a rare genetic mutation she has—began attacking the rest of her body, and more symptoms began to emerge.
As she experienced more autoimmune symptoms, hormonal issues brought her to her OB-GYN, and a thyroid hormone test revealed subclinical hyperthyroidism. Initially, she said she was told to ignore it, but Garner explained that her mother previously had a non-cancerous thyroid nodule, so she wanted further testing out of an abundance of caution. When the testing revealed a nodule, Garner had to fight to get a biopsy, flying home to Austin from the University of Arkansas where she was attending college to ultimately get the care she needed. And when the nodule came back as cancerous, she was in surgery only a week later.
The procedure removed the original nodule on her isthmus and three lymph nodes, and afterward, doctors assured her that she would only need regular checkups. But Garner said her symptoms returned quickly.
This January, she went in for another scan, and one of her lymph nodes raised alarms, and within the month she was scheduled for yet another surgery. Doctors performed a lateral neck dissection and removed the remainder of the left lobe of her thyroid along with 32 lymph nodes, seven of which tested as cancerous.
After the surgery, Garner said she had a drainage tube in her neck for a week, where her neck had been cut open from the top to the middle.
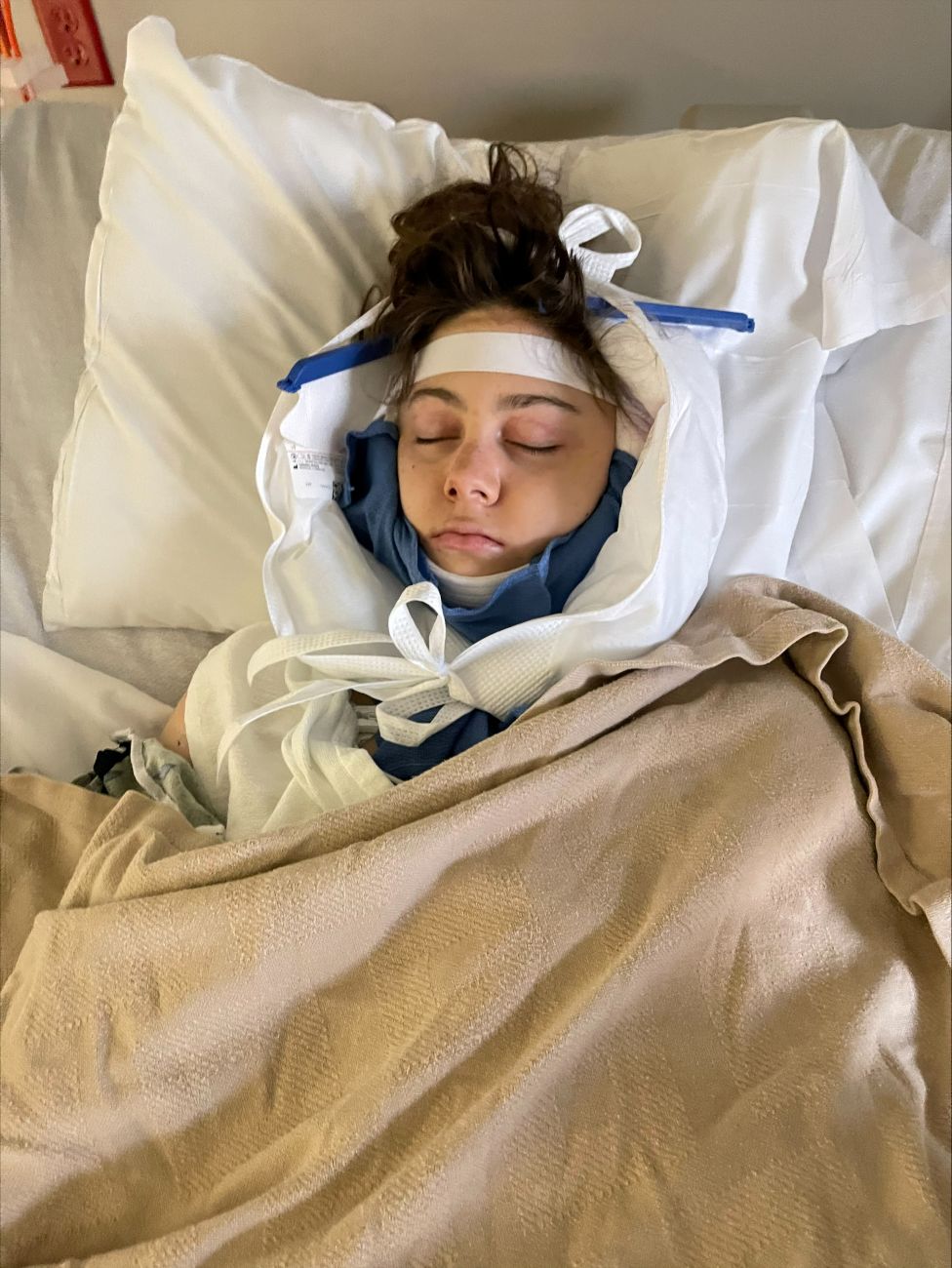
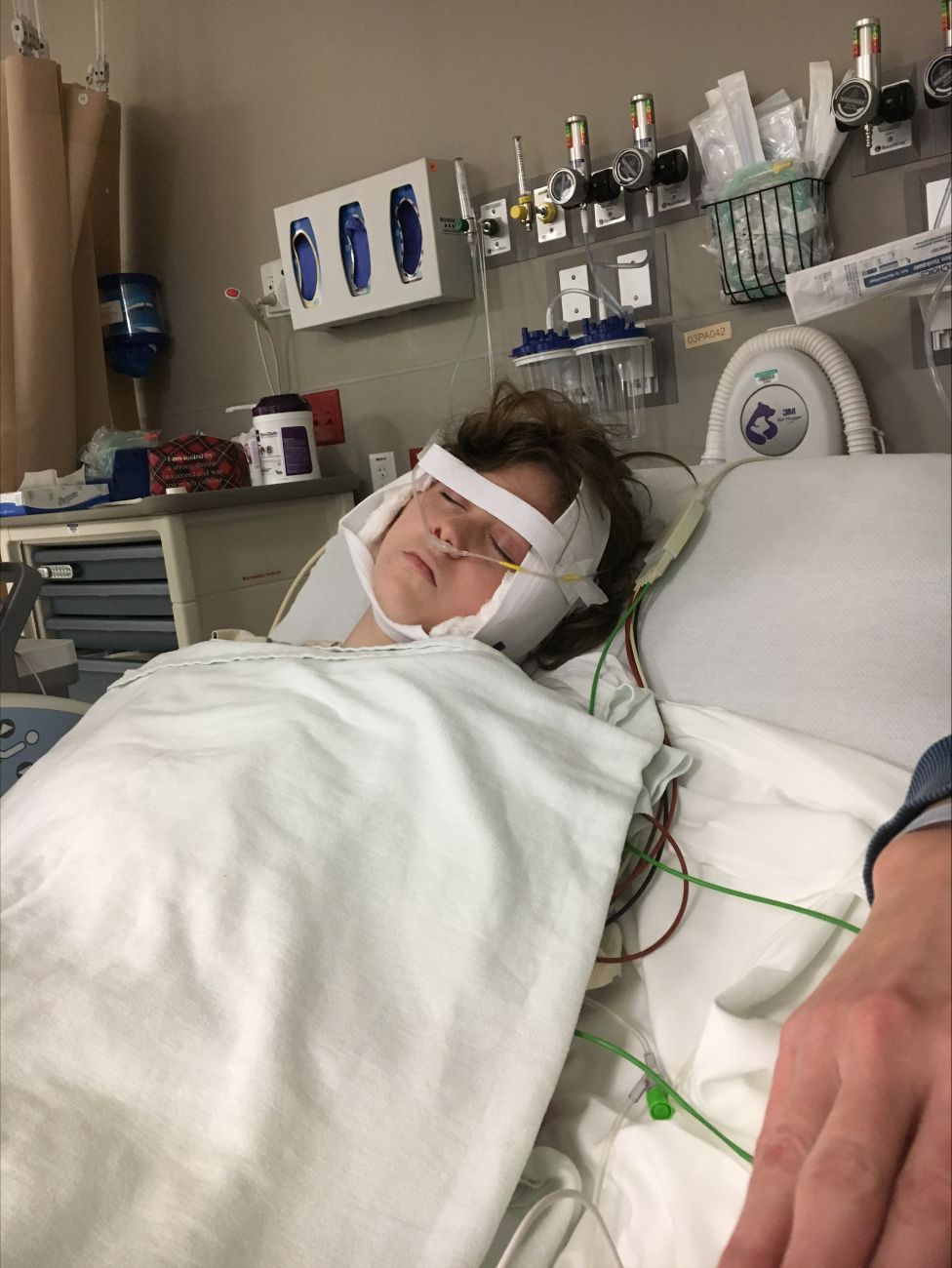
More than two months later, Garner said she does not yet have a full range of motion in her neck and will need physical therapy. She’s also suffering from fatigue as her body adapts to her new hormonal levels.
“As of now, we don’t know where the rest of the cancer could be—if it’s still there [or] if it’s not,” she added.
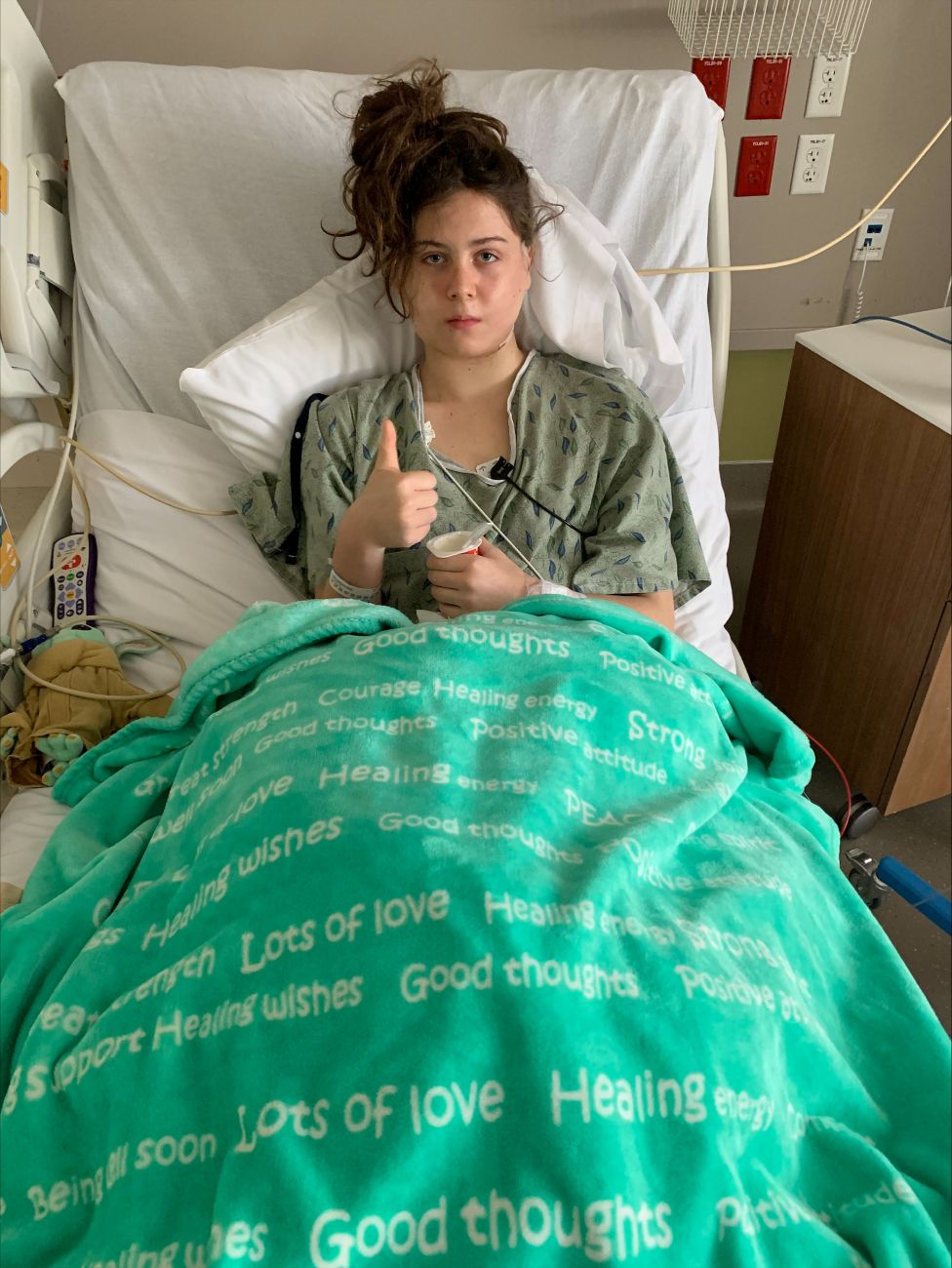
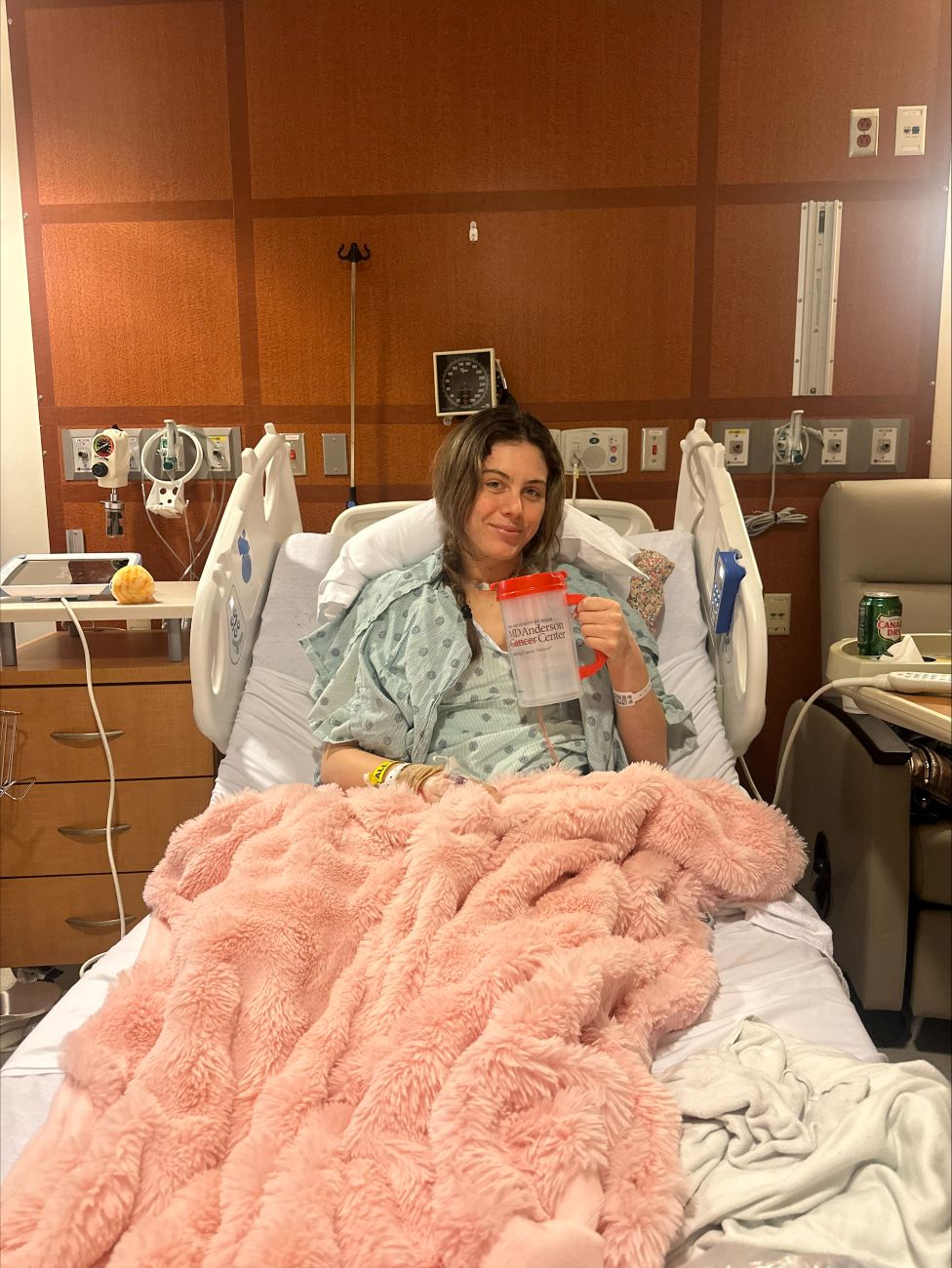
This uncertainty embodies Garner’s entire experience with the healthcare system. At each stage, she’s had to stand up for herself, perform her own research where doctors didn’t have answers, and contend with hospitals and insurance companies as she’s navigated the confusing, opaque healthcare system.
Right now, she’s in yet another back-and-forth with her insurance company after being told she needs new prior authorization for a medication she’s already taking. Garner said she found out from an insurance company patient advocate that the out-of-pocket cost for the monthly shot she needs is $25,000. As a result, she’s had to switch to another medication, her claim has been denied three times, and only half of her needed dosage has been approved.
This is not the first time she’s had to take a less effective medication to get the insurance coverage she needs, either. She explained that her doctors knew she would need a particular medication, but because of fail-first insurance policies, she had to try a series of other medications first.
“I had to start with methotrexate,” she said. “You go on that for about six to eight months, and then you have to prove that it’s not working and your body’s still being attacked [by your immune system]. Then you go to the next one and the next one.”
Garner said she lost count of the number of medications she had to try, but she estimates she went through at least a dozen. By the time her insurance would cover the medication she needed, her jaw joint had already been replaced, and she had irreversible damage in other areas of her body as well.
Garner explained that an anti-competitive and non-transparent environment has contributed to the bureaucracy and high prices that patients like her have to deal with.
“If you can see the prices, it gives the patient, the consumer, the employer an incentive to shop that’ll automatically open the market and force competition,” she said.
Today, Garner is not just a patient but also a reformer, working as a policy analyst with the Texas Public Policy Foundation to advance a more affordable and transparent healthcare system for Americans. It wasn’t until she became involved with healthcare policy that she unraveled and fully understood the system she’s struggled through for so many years.
“I had no idea about cheaper prices or cheaper doctors or different options,” she said, echoing the frustrations many Americans have about the healthcare system.
“I really didn’t want anyone to be how I was: in the dark,” she added. “I was blessed enough to have great parents and good enough insurance while a lot of other people… don’t have that, and they don’t have the resources to advocate for themselves.”